Direct medical care is transforming healthcare delivery in the United States. This model emphasizes direct payments from patients to providers, bypassing traditional insurance. According to a report by the Direct Primary Care Coalition, over 500,000 individuals now benefit from this approach. Dr. John Cullen, a renowned healthcare expert, states, “Direct medical care can address barriers that hinder patient access to quality services.”
The direct medical model promotes transparent pricing and personalized care. Patients appreciate knowing the costs upfront, reducing unexpected medical bills. Data from the American Academy of Family Physicians reveals that 87% of members believe this system enhances patient relationships. However, it is essential to reflect on the limitations. Not everyone can afford direct medical care; accessibility remains a concern.
Moreover, while this model improves care quality, challenges exist. Some providers may struggle with patient volume. This can lead to longer wait times, counteracting the benefits intended by direct medical practices. In summary, the evolution of direct medical care presents exciting prospects and significant challenges within the healthcare landscape.
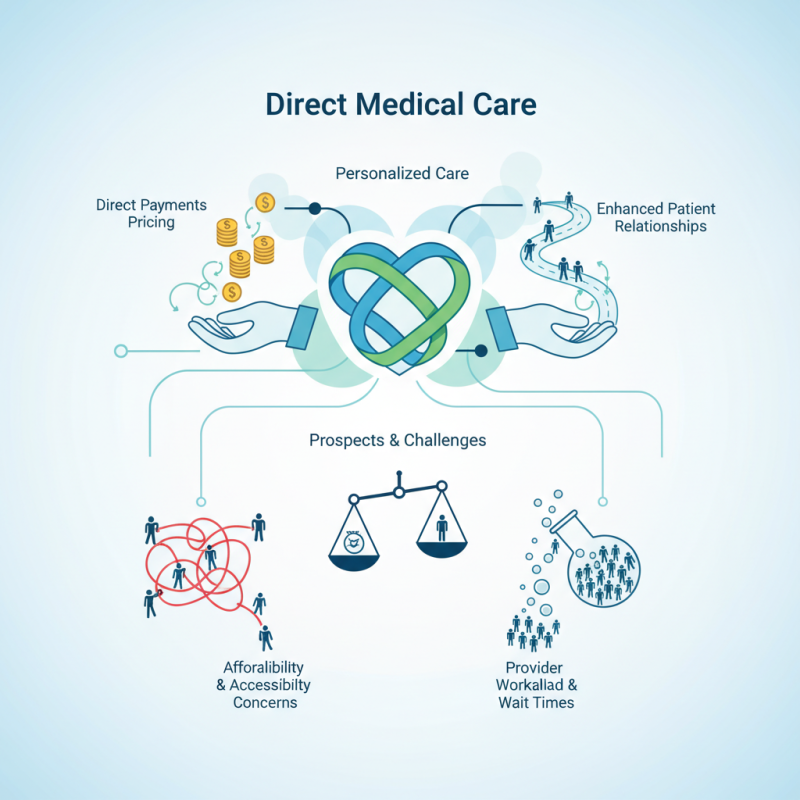

Direct Medical Care (DMC) is an innovative approach to healthcare that focuses on delivering services directly to patients without involving third-party insurers. This model allows for fewer administrative hassles and lower overhead costs. According to the Direct Primary Care Coalition, around 500,000 patients in the U.S. are currently enrolled in DMC models. This figure highlights a growing trend towards personalized care and efficient healthcare delivery.
DMC operates on a simple premise: patients pay a monthly fee directly to healthcare providers. This arrangement encourages transparent pricing, allowing patients to understand their healthcare costs upfront. Reports show that DMC can save patients up to 40% on annual medical expenses. However, not all patients may find this model suitable. Some may struggle with the idea of regular payments for services they might not use every month.
Quality of care is often cited as a major benefit of DMC. Providers typically have more time to spend with each patient, fostering stronger relationships. Yet, there is a downside. Some critics argue that DMC can create a divide, favoring those who can afford to pay out of pocket. The challenge remains in how to make DMC accessible for all individuals, regardless of their financial situation. Balancing affordability and quality care requires ongoing conversation and evaluation within the healthcare community.
Direct Medical Care (DMC) is emerging as a significant trend in healthcare. This model primarily focuses on direct patient-provider interactions, bypassing traditional insurance complexities. Numerous studies, including data from the American Academy of Family Physicians, show that over 50% of patients prefer this model due to its transparency and affordability.
Key features of DMC include a subscription-based payment structure. Patients pay a fixed monthly fee for comprehensive services. This often covers routine check-ups, lab tests, and urgent care. Research indicates that practices utilizing DMC can reduce administrative costs by as much as 30%. This allows healthcare providers to focus more on patient care.
Another essential aspect is accessibility. DMC practices often offer extended hours and easier communication methods. Providers can engage with patients more directly through digital platforms. However, there are challenges, such as limited coverage for specialized services. Patients might still need traditional insurance for serious conditions. Understanding these limitations is crucial for making informed healthcare choices.
Direct Medical Care (DMC) presents a distinct approach compared to traditional healthcare models. Under DMC, patients often pay a monthly fee directly to providers. This bypasses insurance intermediaries, reducing administrative overhead. According to a 2020 report from the Direct Primary Care Coalition, over 1.4 million patients are now served through this model in the United States, demonstrating its growing acceptance.
A key difference lies in accessibility and care personalization. Traditional healthcare systems often limit appointment time, with average visits lasting just 15 minutes. DMC allows longer visits, fostering better doctor-patient relationships. In fact, studies show that patients in DMC feel more satisfied with their care. Data from Health Affairs indicates a 30% improvement in patient satisfaction rates in DMC settings compared to traditional models. However, this model isn't perfect. Limitations in service scope and potential inconsistency in provider quality can lead to concerns for some patients.
Another factor is cost transparency. In traditional systems, bills can come as a surprise. DMC aims to provide clear pricing up front, which can help manage patient expectations. Yet, the shift to direct payment may pose challenges for individuals without the means to pay upfront. This financial barrier raises questions about equity in healthcare access.
| Aspect | Direct Medical Care | Traditional Healthcare |
|---|---|---|
| Payment Model | Monthly membership fees | Fee-for-service payments |
| Access to Providers | Direct communication with doctors | Through insurance networks |
| Appointment Scheduling | Same-day or next-day availability | Typical wait times may vary |
| Cost Transparency | Clear upfront pricing | Variable costs depending on insurance |
| Patient Volume | Lower patient load | Higher patient volume |
| Services Offered | Basic and preventative care | Comprehensive healthcare services |
| Follow-up Care | Ongoing patient monitoring | Limited direct follow-up |
Direct medical care (DMC) offers a fresh perspective on healthcare access. By eliminating the middleman, patients enjoy direct interactions with their healthcare providers. This model enhances communication, making it easier for patients to address their concerns directly.
One major benefit of DMC is cost transparency. Patients often find they can predict expenses without hidden insurance fees. This clarity helps in budget planning and reduces stress. Additionally, DMC allows for longer appointment times. Patients receive more attention, ensuring thorough discussions about their health concerns.
Tip: Be proactive about your health. Regular check-ups can prevent bigger issues later.
Tip: Research providers to find one that fits your timelines and needs. Direct medical care may not be available everywhere, so local availability matters.
Direct Medical Care (DMC) is emerging as a viable solution in the healthcare landscape. It offers patients direct access to care without the need for insurance. The appeal lies in the transparency of costs and the simplicity of services. According to the Direct Primary Care Coalition, about 25% of primary care physicians practice DMC, signaling a shift towards more patient-centered models. This approach may address some systemic issues.
The experience of patients in DMC is often positive. Many report higher satisfaction levels compared to traditional models. A report from the Physicians Foundation indicates that 71% of doctors practicing DMC feel they can provide better care. However, the model is not without challenges. Accessibility remains a concern. Many potential patients may still rely heavily on insurance. The financial implications could limit its expansion.
Looking ahead, DMC could reshape how healthcare functions. The recent surge in telemedicine usage during the pandemic showcases a growing acceptance of alternative care models. Yet, the sustainability of DMC hinges on broader recognition and acceptance. Stakeholders need to address the barriers in communication around this model. Further research is necessary to gauge its long-term impact on healthcare delivery.



2382 Faraday Avenue, Ste 300
Carlsbad, CA 92008
The materials on this website are for your general educational information only. Information you read on this website cannot replace the relationship that you have with your healthcare professional. We do not practice medicine or provide medical services or advice as a part of this website. You should always talk to your healthcare professional for diagnosis and treatment.
©2025 Breg, Inc. All rights reserved. All trademarks and registered trademarks are owned by the copyright holder.